I'm afraid to drive. When I'm reading, part of a sentence can just disappear! I have to look at things "out of the corner of my eye" in order to see them well. These visual problems are associated with a condition called "macular degeneration".
Macular degeneration is the most common cause of visual problems in people over the age of 50. Its onset is typically so gradual people may not realize that they have a problem even when it has a significant impact on their everyday life. Some of the symptoms are listed above. In general there is a loss of "precise" vision in the central area of a person's "visual field" (the entire area seen by the eye).
What is the macula?
The macula is a small, highly sensitive area of the retina. It produces the crisp, precise image that we depend on in order to read, drive and perform other tasks that require us to distinguish details. The cells that are specific for color vision (cones) are packed into this area.
Even though your central vision is impaired, your side or peripheral vision is not. This means you may be able to see the outline of a clock but still not be able to see the hands that allow you to tell the time.
What is Age-Related Macular Degeneration?
When the macula is not functioning properly your central vision may appear, fuzzy, hazy and distorted. The most common cause of this is "age related macular degeneration." There are two different processes that can cause macular degeneration.
-
Dry macular degeneration
This is the most common type (90%) of macular degeneration. As a person ages tiny whitish yellow mounds composed of complex proteins and fats form under the retina. These are called drusen. Most people over 40 have some drusen deposits present; however, some people as they age accumulate a substantial amount of drusen in the area of the macula. This interferes with the function of the vision cells and ultimately can compromise the specialized mission of the macula (visualization of a fine, detailed image). Dry macular degeneration generally develops slowly and takes many years before significant visual impairment occurs.
-
Wet (exudative) macular degeneration
Although both types of macular degeneration feature drusen, wet (exudative) macular degeneration features an additional complication. New blood vessels also form in a layer under the macula. These blood vessels can break open and leak blood and fluid into the surrounding tissue. This tissue becomes scarred as the body attempts to seal off the leaking vessels. The resulting visual loss can occur quite rapidly and be much more severe than that seen in the more typical form of macular degeneration.
How is macular degeneration diagnosed?
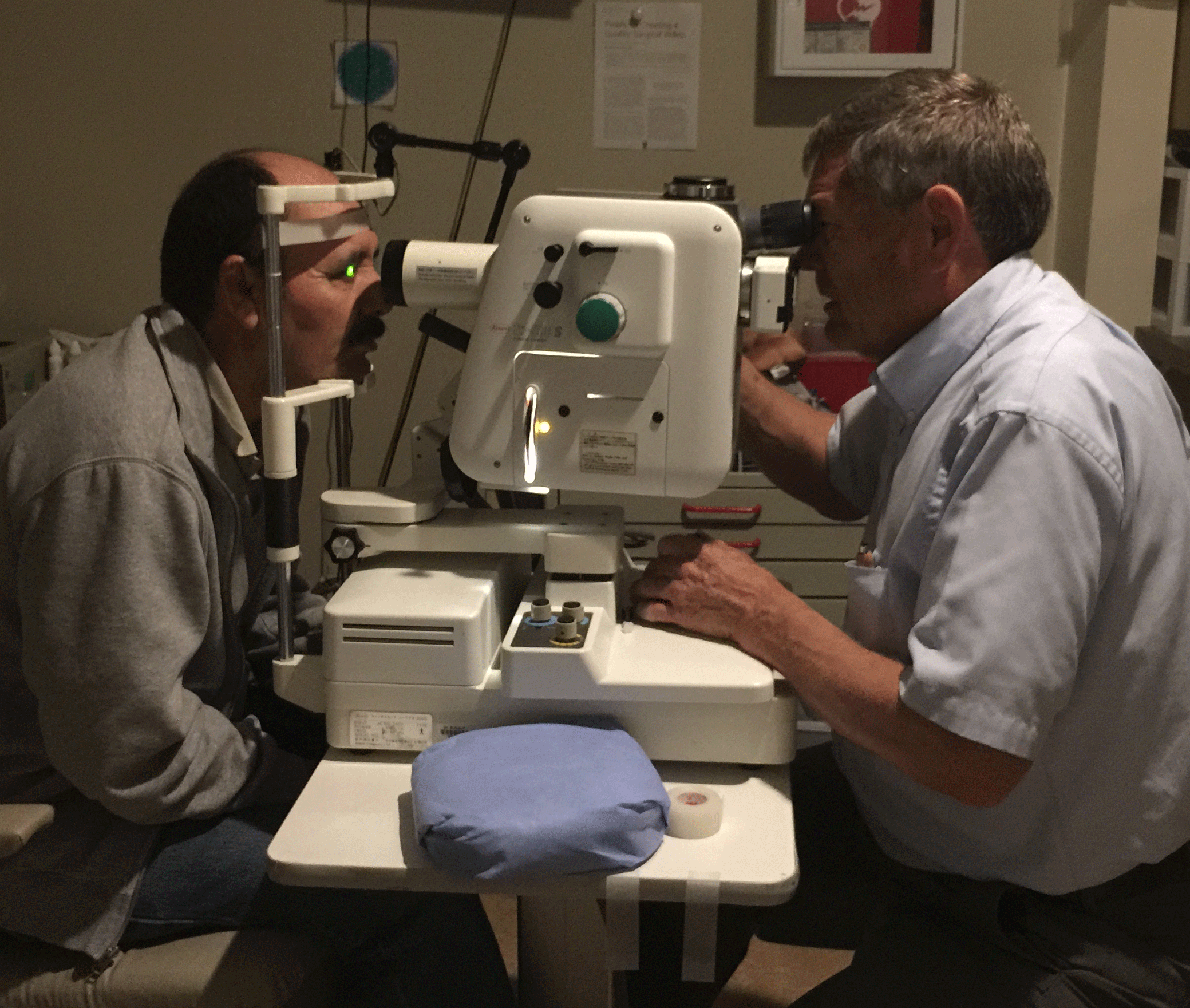
Ophthalmologists use a variety of techniques to diagnose macular degeneration. An ophthalmoscope (lighted instrument) is used to examine the retina. In addition, some special tests may be administered. The Amsler Grid test is used to detect blind spots or distortion of central vision. This test is also used to monitor patient visual perception. If you are diagnosed with macular degeneration you should perform a visual check daily using the Amsler Grid test.

Instructions for use:
-
Perform the test in bright light.
-
If you wear reading glasses put them on.
-
View the grid at arms length and cover one eye. With the uncovered eye, stare at the black dot in the center of the grid.
-
During the entire test, having one eye covered, stare at the center of the grid
-
Cover the eye you just tested and repeat the test with the other eye.
-
If any area of the grid looks abnormal or more indistinct compared to previous tests contact your ophthalmologist.
Color vision test is used to see if the patient can detect letters or symbols camouflaged in colored patterns.
Optical coherence tomography (OCT) can be used to diagnose and monitor the progression of AMD. At Sunalp Laser Vision we use the newest model of OCT, NIDEK-RS 300
Fluorescein Angiography (FA) may be performed to further evaluate for any leaking blood vessels.
How is macular degeneration treated?
Laser treatments and NEW medications
There are a variety of ways to treat wet macular degeneration, all designed to prevent further progression. Sunalp Laser Vision offers state-of-the-art services for both types of macular degeneration.
Laser treatments
Laser treatments can slow vision loss from AMD and in some cases improve vision. Laser treatments can seal leaky blood vessels to reduce scaring that could decrease the central vision.

Anti-VEGF therapy
At Sunalp Laser Vision we use a highly successful treatment protocol involving use of a drug that impairs the production of new blood vessels. This class of drugs is called vascular endothelial growth factor (VEGF) inhibitors or anti-VEGF. In addition we use an innovative method of introducing this drug into the eye. This method was developed by Dr. Sunalp to specifically avoid many of the complications associated with introducing the drug into the eye. This treatment technique, which minimizes side effects while maximizing treatment benefits, is one of the many ways Sunalp Laser Vision has demonstrated commitment to state-of-the-art services.

Standard Approach
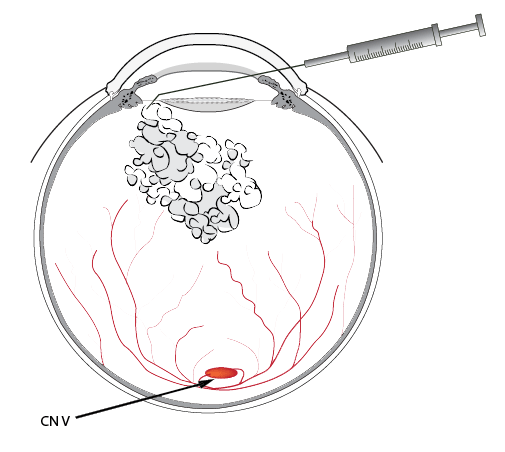
Dr. Sunalp's Perilimbic Approach
Why choose Dr. Sunalp?
-
Dr. Sunalp pioneered a NEW and SAFER AVASTIN injection technique
-
Highly experienced physician
-
Trained at University of Southern California (USC)-top 10 in the USA
-
Board certified physician
-
Dr. Sunalp is a diplomat of the American Board of Ophthalmology, a Fellow of the American Academy of Ophthalmology, Fellow of the Royal College of Ophthalmology, England and a Fellow of the American College of Surgeons
-
We use state-of-art diagnostic equipment (The newest: NIDEK-RS 300)
-
Fluorescein Angiography (FA)
-
Argon Laser in-house treatment
-
FDA approved implantable telescope for End-Stage Age-Macular Degeneration
News on Age-Related Macular Degeneration Treatment!
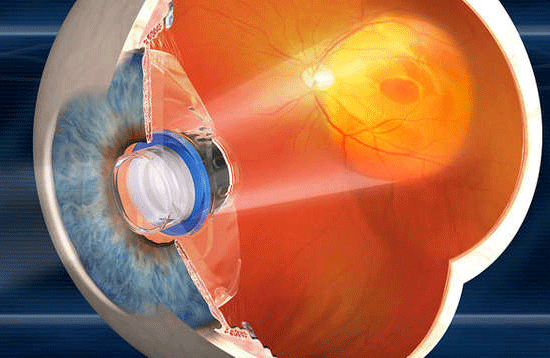
Implantable Telescope: A solution for end stage macular degeneration
The tiny telescope implant, developed by VisionCare Ophthalmic Technologies, Inc. and approved by Food and Drug Administration for people over 65, now available at Sunalp Laser Vision.
An implantable tiny telescope, about the size of a pea, is implanted inside one eye behind the iris (the colored part of the eye) to improve vision and quality of life for the patient with the most advanced form of macular degeneration: End Stage AMD
Please call us at (559) 688-2020 to schedule an appointment with Dr. Sunalp and see if you are eligible candidate for the Implantable Telescope.
Nutritional supplementation
Although there is no "cure' for dry macular degeneration there are some strategies that appear to be successful in preventing progression to the more severe "wet" type. One of these has been evaluated in a study called Age-Related Eye Disease Study 2 (AREDS2). This study showed that the following supplements reduced the risk of disease progression in those with high risk for developing late-stage, or wet, macular degeneration.
-
Vitamin C – 500 mg
-
Vitamin E – 400 IU – 10 mg
-
Zeaxanthin – 2 mg – 80 mg
-
Copper (as cupric oxide) – 2 mg
Other studies have shown the importance of foods rich in lutein and zeaxanthin. These include dark leafy greens such as broccoli, brussels sprouts, lettuce, spinach, and Swiss chard. Other studies have shown benefits of beta-carotene. This is found in yellow and orange foods such as sweet potatoes, butternut squash and, yes carrots
Prevention is the best medicine
Regular eye exams are the most important in early detection of macular degeneration, as the symptoms of the disease often go unnoticed.



